The big picture
Safety is preparation, not prohibition
🔬
What the research actually says about adverse events
A 2024 systematic review in JAMA Psychiatry (Hinkle et al., 581 clinical trial participants) found classic psychedelics were generally well-tolerated in supervised settings — the most common adverse events were transient blood pressure elevation, nausea, and anxiety during sessions. Serious adverse events were rare and significantly more common in recreational than clinical settings. The safeguards matter: screening, preparation, a trained provider present, and integration support are not bureaucratic boxes — they are the mechanism by which risk is managed.
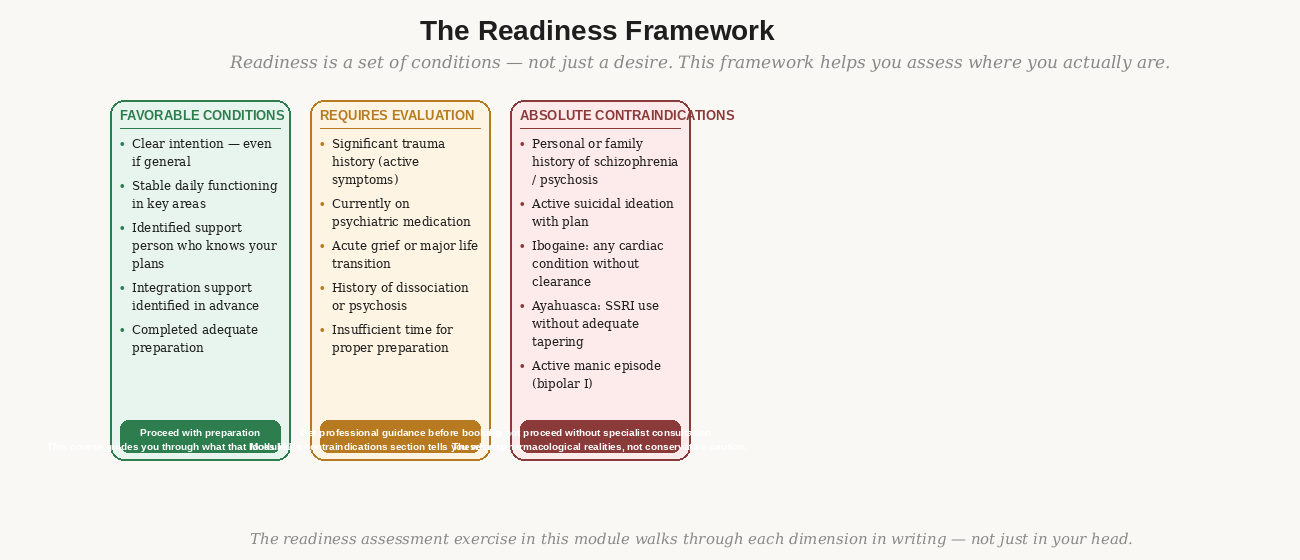
The readiness framework — three zones from favorable conditions through absolute contraindications. Click to enlarge.
The safety landscape differs significantly by substance. Psilocybin and LSD have relatively benign physiological profiles in healthy adults — the main risks are psychological and context-dependent. MDMA carries cardiovascular and thermoregulatory risks. Ibogaine has the most serious safety profile and requires medical supervision in a clinical setting. Ketamine, as a legal medicine with established dosing protocols, has the most refined safety infrastructure of any substance on this page.
The contraindications on this page are drawn from clinical trial exclusion criteria, expert consensus statements (including the 2024 US National Network of Depression Centers consensus on psilocybin), and pharmacological research. They represent the current state of evidence — many will evolve as research expands into more diverse populations.
Quick reference
Risk by medicine and concern area
| Medicine |
Psychosis history |
SSRI interaction |
Cardiac risk |
Pregnancy |
Lithium combo |
| 🍄 Psilocybin |
High ⚠ |
Blunts effect |
Low |
Unknown |
Seizure risk |
| 🔬 MDMA |
Moderate |
Fully blocked |
High ⚠ |
Unknown |
Caution |
| 🌿 Ayahuasca |
High ⚠ |
Serotonin syn. |
Moderate |
Avoid |
Seizure risk |
| 🌱 Ibogaine |
High ⚠ |
Caution |
QTc ⚠ High |
Avoid |
Avoid |
| 🔭 LSD |
High ⚠ |
Blunts effect |
Low |
Unknown |
Seizure risk |
| 💉 Ketamine |
Use caution |
No interaction |
Low–mod |
Unknown |
Generally safe |
This matrix reflects general clinical guidance, not absolute rules. Individual circumstances, comorbidities, and provider expertise can change the risk calculus. Always consult a physician with psychedelic expertise — not a general practitioner.
Mental health history
Psychiatric contraindications
Psychiatric history is the most important screening area in psychedelic therapy. The conditions below don't necessarily mean no access to any treatment — they mean that the right medicine, the right setting, and close psychiatric oversight become critical variables.
⛔ Strong contraindication
Personal history of psychosis, schizophrenia, or schizoaffective disorder
This is the most consistent exclusion criterion across all clinical trials. Classic psychedelics activate 5-HT2A receptors in a way that can precipitate or worsen psychotic symptoms — including in people who have been stable for years. A single psychedelic episode has triggered persistent psychosis in vulnerable individuals. The risk is considered too high to navigate with preparation or dosing adjustments alone.
Exception: Ketamine operates through a different mechanism (NMDA antagonism) and has a different risk profile. Ketamine may still be considered under close psychiatric supervision, though caution applies.
⛔ Strong contraindication
First-degree family member with schizophrenia or psychotic disorder
A genetic predisposition to psychosis — even without a personal episode — is treated as a significant risk factor across clinical trial protocols. The biological substrate for vulnerability may be present even if it has never been activated. Most research protocols exclude people with a first-degree relative (parent, sibling, child) with schizophrenia or schizoaffective disorder. This is a precautionary position; it may evolve as the field learns more about who is actually at risk versus who has the genetic variant without functional vulnerability.
⚠ Significant caution
Active bipolar I disorder or current manic episode
Classic psychedelics can trigger manic episodes in people with bipolar I, particularly during or immediately after a session. This is one of the more nuanced areas — bipolar II, cyclothymia, and well-stabilized bipolar I with long periods of mood stability may have different risk profiles. The key variables are: how stable is the person currently, what is the polarity of any current mood state, and what does a qualified psychiatrist recommend?
People with bipolar II who are currently euthymic and medically stable have been included in some trials. This requires individual evaluation with a psychiatrist who knows your history, not self-assessment.
⚠ Significant caution
Active suicidality with intent or plan
Active suicidal ideation with a specific intent or plan is a contraindication for retreats and most outpatient psychedelic settings — not because psychedelics worsen suicidality, but because the appropriate level of care is inpatient psychiatric monitoring, not a psychedelic session. Passive suicidal ideation (wishing one were dead, without a plan) is handled differently across protocols and is often included in trials where depression is the target indication. Ketamine specifically has FDA approval for MDD with acute suicidal ideation in monitored settings.
◈ Nuanced — evaluate carefully
Personality disorders (especially Cluster B)
Borderline, narcissistic, and antisocial personality disorders present meaningful risks in psychedelic contexts — primarily around destabilization of emotion regulation, transference issues with facilitators, and difficulty integrating challenging content. This is not a blanket contraindication. Many people with BPD have benefited from psychedelic work with appropriate support. The quality of the therapeutic relationship, provider experience with complex presentations, and integration support are decisive factors.
◈ Nuanced — evaluate carefully
Dissociative disorders
Dissociation during psychedelic experiences is common and generally temporary. But people with chronic dissociative disorders (DPDR, DID, structural dissociation) may find that psychedelics intensify dissociative states rather than resolving them — at least without a very specific and expert therapeutic frame. Some practitioners specialize in this intersection. Ketamine's dissociative mechanism is a particular consideration for people already prone to dissociation.
✓ Generally navigable
Depression, PTSD, anxiety, OCD, addiction
These are the primary
indications for psychedelic therapy in clinical research — not contraindications. People with these conditions are the target population for the most significant trials. Medication management (particularly SSRIs — see below) and severity level are the key variables to discuss with a provider, not the diagnoses themselves.
Exception: Very severe, acute presentations with high instability may require stabilization before psychedelic work. Timing and readiness matter.
✓ Generally navigable
Trauma history, including complex PTSD
Trauma history — including severe or complex trauma — is not a contraindication. MDMA-assisted therapy for PTSD specifically targeted people with severe, treatment-resistant trauma. Preparation quality, facilitator trauma training, and integration support are the critical factors. More complex trauma presentations simply require more careful provider selection and preparation, not exclusion.
Drug interactions
Medication interactions — by drug class
This is the area of greatest practical complexity for most people seeking psychedelic therapy. The interactions below range from "reduces effectiveness" to "potentially life-threatening." Full medication disclosure to any provider is non-negotiable — including supplements, herbal preparations, and as-needed medications.
⚠️
Never taper or stop psychiatric medications without medical supervision. Stopping antidepressants abruptly can cause discontinuation syndrome and worsen the conditions they were treating. If you're considering psychedelic therapy and are on psychiatric medications, this conversation must happen with a prescribing physician or psychiatrist — not a facilitator, retreat center, or this website.
💊
SSRIs and SNRIs
Prozac, Zoloft, Lexapro, Effexor, Cymbalta, Pristiq + others
| Substance | Interaction | Severity |
|---|
| Psilocybin / LSD |
SSRIs downregulate 5-HT2A receptors — reducing or blunting psychedelic response. Evidence is mixed on severity; some people on SSRIs report near-complete blockade, others report partial effect. Research is actively investigating. Does not create a dangerous combination, but may severely limit therapeutic benefit. |
Effect reduced |
| MDMAEspecially SSRIs |
Controlled studies confirm SSRIs and SNRIs essentially fully block MDMA's empathogenic effects. The stimulant component persists but the therapeutic mechanism is lost. Combining MDMA with SSRIs/SNRIs for therapeutic purposes is generally not indicated. Does not create a danger if accidentally combined, but renders treatment ineffective. |
Fully blocked |
| Ayahuasca |
Ayahuasca contains MAOIs. Combining any serotonergic drug — including SSRIs — with an MAOI creates risk of serotonin syndrome, a potentially life-threatening condition. SSRIs must be fully cleared before any ayahuasca ceremony. Clearance time varies by drug: fluoxetine (Prozac) has a very long half-life and may require 4–6 weeks. |
Serotonin syndrome risk |
| Ketamine |
No dangerous interaction with SSRIs. Ketamine operates through NMDA antagonism, not serotonergic pathways. SSRIs do not significantly alter ketamine's effects. This is one reason ketamine is the most accessible psychedelic-adjacent treatment for people currently on antidepressants. |
No interaction |
⚡
MAOIs (Monoamine oxidase inhibitors)
Phenelzine, tranylcypromine, selegiline — also found in ayahuasca itself (Banisteriopsis caapi vine)
| Substance | Interaction | Severity |
|---|
| MDMA + MAOI |
The most dangerous combination on this page. MAOIs prevent breakdown of serotonin and the stimulant metabolites of MDMA, causing massive accumulation of serotonergic activity. Serotonin syndrome: fever, agitation, muscle rigidity, seizures. Fatalities have occurred. This combination must never happen. |
⛔ Life-threatening |
| Psilocybin / LSD + MAOI |
At typical therapeutic doses, combining with an MAOI may intensify and prolong the psychedelic experience. Some practitioners use low-dose MAOIs intentionally to potentiate psilocybin, but this is specialist territory requiring precise dosing. At higher doses or without expert guidance, the combination can produce dangerously prolonged and overwhelming experiences. |
High — expert only |
| Ayahuasca note |
Ayahuasca contains an MAOI (the Banisteriopsis caapi vine). Anyone taking MAOI antidepressants should not take ayahuasca — the additive MAOI effect plus DMT creates extreme risk. Additionally, anyone taking any serotonergic drug before ayahuasca is at risk through the MAOI component in the brew itself. |
⛔ Avoid completely |
🔋
Lithium
Lithium carbonate, lithium orotate — used for bipolar disorder and depression augmentation
| Substance | Interaction | Severity |
|---|
| Classic psychedelics + LithiumPsilocybin, LSD, DMT, ayahuasca |
Analysis of case reports and survey data shows a consistent signal: combining lithium with classic psychedelics significantly increases seizure risk. The mechanism is not fully understood. Reports include multiple cases of grand mal seizures following the combination. This is not a theoretical concern — enough cases exist that it represents a real clinical warning. Lithium is a contraindication for classic psychedelic use. |
⛔ Seizure risk |
| Ketamine + Lithium |
Some caution advised; lithium may affect ketamine's antidepressant mechanism and alter dissociative effects. Not as clearly dangerous as lithium + classics. Requires monitoring. Clinical providers administering ketamine to people on lithium generally do so with careful oversight. |
Caution — monitor |
❤️
QTc-prolonging medications
Many antipsychotics, some antibiotics, antifungals, antihistamines — check your full medication list
| Substance | Interaction | Severity |
|---|
| Ibogaine + QTc drugsHaloperidol, methadone, azithromycin, many others |
Ibogaine itself significantly prolongs the QTc interval (a measure of electrical heart rhythm). Combining it with any other QTc-prolonging drug is dangerous and has been associated with cardiac arrest and death. Ibogaine clinics require a 12-lead ECG before treatment and a complete medication review. Any QTc-prolonging drug must be cleared before ibogaine, and baseline QTc must be within safe limits. |
⛔ Cardiac arrest risk |
| MDMA + QTc drugs |
MDMA increases heart rate and blood pressure substantially. Adding QTc-prolonging drugs increases cardiovascular risk. Less immediately dangerous than ibogaine combinations, but a genuine concern for people with any cardiac vulnerability. |
Elevated cardiac risk |
📋
Other medications requiring attention
Stimulants, antipsychotics, anticonvulsants, tramadol, St. John's Wort
| Medication | Interaction | Severity |
|---|
| AntipsychoticsRisperdal, Seroquel, Abilify, Zyprexa |
Antipsychotics largely block or significantly blunt classic psychedelic effects (5-HT2A antagonism). Concurrent use renders most classic psychedelic therapy ineffective. Atypicals also prolong QTc — relevant for ibogaine. For people on antipsychotics for psychiatric stability, discontinuing them is a significant clinical decision. |
Blocks effect / QTc concern |
| StimulantsAdderall, Ritalin, Vyvanse, modafinil |
Additive cardiovascular effects with MDMA — increased heart rate and blood pressure, potential for hyperthermia. Lower concern with classic psychedelics. Generally, stimulants should be avoided on days involving MDMA or high-dose psilocybin/LSD. Low-dose stimulants with psilocybin therapy are less clearly dangerous but unnecessary. |
MDMA: cardiovascular risk |
| Tramadol |
Tramadol has serotonergic activity — combining it with MDMA or ayahuasca (MAOI) increases serotonin syndrome risk. Often overlooked because it's classified as an opioid; its serotonergic mechanism is the relevant concern here. Must be disclosed to any psychedelic provider. |
Serotonin syndrome risk with MDMA |
| St. John's WortHypericum perforatum |
A commonly overlooked serotonergic supplement. Combines dangerously with MDMA and ayahuasca (MAOI). Must be disclosed — people often don't mention herbal supplements. Clearance time: typically 1–2 weeks after stopping. |
Serotonin risk — disclose always |
| Anticonvulsants / Mood stabilizersValproate, lamotrigine, carbamazepine |
Lamotrigine appears not to share lithium's seizure risk with psychedelics based on case reports. Valproate and carbamazepine are more complex — their anticonvulsant effects may actually reduce some risks but their full interaction profile with psychedelics is not well studied. Individual evaluation with a prescriber is essential. |
Evaluate individually |
💡
The washout problem. Many medications take days to weeks to fully clear the body. Fluoxetine (Prozac) has an active metabolite with a half-life of 1–2 weeks — full clearance may take 4–6 weeks. Any discussion with a provider about stopping a medication to pursue psychedelic therapy needs to account for: discontinuation syndrome risks, psychiatric stability during the taper, who is medically supervising the process, and what safety net is in place. This is not something to manage alone or quickly.
Medical history
Physical health contraindications
Physical health concerns are generally more substance-specific than psychiatric ones. The right medicine for the right person — with appropriate medical screening — often remains accessible even with significant medical history.
⛔ High risk — ibogaine and MDMA
Serious cardiovascular conditions
MDMA significantly elevates heart rate and blood pressure, increasing cardiac workload. Ibogaine causes QTc prolongation — a dangerous electrical rhythm change. For people with uncontrolled hypertension, arrhythmias, structural heart disease, recent cardiac events, or prolonged baseline QTc: MDMA and ibogaine are high-risk or contraindicated. Psilocybin and ketamine have significantly milder cardiovascular profiles and may remain accessible with monitoring.
⛔ All substances
Pregnancy and breastfeeding
No psychedelic substance has adequate human safety data for pregnancy. The precautionary principle applies: avoid all psychedelic experiences — including microdosing — during pregnancy and while actively trying to conceive. The absence of evidence of harm is not the same as evidence of absence of harm. Breastfeeding introduces the additional concern of drug transfer to an infant. This is a firm recommendation, not a nuanced one.
⚠ Significant caution — ibogaine
Liver disease
Ibogaine is extensively metabolized by the liver. Significant liver disease or impairment may affect ibogaine clearance unpredictably, increasing risk of cardiac events. Liver function testing before ibogaine is standard at responsible clinics. Psilocybin and other classics are less dependent on hepatic metabolism and generally better tolerated with liver conditions.
⚠ Caution — all substances
Uncontrolled hypertension
Classic psychedelics produce modest, transient blood pressure increases. MDMA produces more substantial increases. For people with blood pressure that is well-controlled on medication, the risk is generally lower. For those with uncontrolled hypertension, even a transient spike during a session carries meaningful risk. Blood pressure monitoring during sessions is standard practice in clinical settings.
◈ Nuanced
Epilepsy and seizure disorders
Classic psychedelics are not reliably proconvulsant in people without the lithium combination risk factor. Small numbers of people with stable, well-controlled epilepsy have participated in psychedelic research. However, the combination of high doses, physiological stress, and sleep disruption associated with intense sessions can theoretically lower seizure threshold. Evaluation with a neurologist is indicated. Ketamine may be a safer option for some people with seizure disorders.
◈ Nuanced
Significant visual or hearing impairment
Not a contraindication, but a relevant consideration for session planning and safety. People who use hearing aids need to consider how an extended session affects device management and communication with the facilitator. Eyemask-based protocols (standard in most clinical settings) are accessible regardless of visual status. Facilitators working with people with sensory impairments need to adapt their protocol accordingly.
Per substance
Medicine-specific safety profiles
Each substance on this page has a distinct risk profile. Understanding what's specific to each medicine matters — a contraindication for ibogaine is not a contraindication for psilocybin.
🍄
Psilocybin
Classic psychedelic · 4–6 hour duration · Oral
Overall safety profile
Favorable in clinical settings
Avoid or strong caution
Personal/family history of psychosis
Active bipolar I / manic episode
Proceed with care
Antipsychotics (blocks effect)
Active suicidality with plan
Personality disorders (complex)
Generally safe with monitoring
Depression / anxiety / PTSD
Stable cardiovascular conditions
Most seizure disorders (evaluate)
📋 Key screening: Psychiatric history including family history, full medication list, baseline blood pressure. Most cardiac conditions do not preclude psilocybin. The 2024 NNDC consensus statement notes the physiological safety profile in supervised settings is strong; psychological risk management is the primary focus.
🔬
MDMA
Empathogen · 3–5 hour duration · Oral
Overall safety profile
Moderate — cardiovascular caution
Avoid or strong caution
MAOI medications (life-threatening)
Significant cardiac disease
Uncontrolled hypertension
Proceed with care
SSRIs / SNRIs (fully blocked — ineffective)
Stimulants (cardiovascular risk)
Generally safe with monitoring
Off medications or cleared
📋 Key screening: Full cardiovascular evaluation including ECG, blood pressure, complete medication review. MDMA is not FDA approved (as of 2024); clinical access is through trials. Most safety data comes from the MAPS Phase 3 trial protocol, which included 2-hour post-session monitoring as standard.
🌱
Ibogaine
Atypical psychedelic · 24–36 hour duration · Oral
Overall safety profile
Requires medical setting — highest risk
Avoid or strong caution
Prolonged QTc at baseline (≥450ms)
Any QTc-prolonging medication
Significant liver disease
Opioids (before full medical clearance)
Proceed with care
Any psychiatric comorbidity
Possible with rigorous screening
Opioid use disorder (primary indication)
PTSD — Stanford 2024 study
Normal cardiac baseline + ECG
📋 Key screening: 12-lead ECG mandatory, potassium and magnesium levels, liver function tests, complete medication history, cardiac stress testing for higher-risk individuals. Ibogaine-associated deaths are real but almost exclusively linked to inadequate screening and unsupervised use. A responsible clinic's protocol dramatically reduces this risk.
💉
Ketamine
Dissociative anesthetic · 45 min–2 hrs · IV / IM / intranasal
Overall safety profile
Well-established · Most accessible
Avoid or strong caution
Uncontrolled hypertension (raises BP)
Active psychosis or mania
History of ketamine dependence
Safe — key advantage cases
People on SSRIs / antidepressants
Available in all 50 states legally
📋 Key advantage: Ketamine is the only FDA-approved psychedelic-adjacent treatment and does not interact with SSRIs. It is the most clinically accessible option for people who are currently on antidepressants, have psychiatric family history that precludes classics, or cannot travel to Oregon/Colorado. Its safety infrastructure is the most established of any substance on this page.
Pathways forward
Who can still access care when classics are restricted
Many people encounter something on the contraindication lists above and conclude psychedelic therapy is off the table. Often it isn't — there's a different medicine, a different protocol, or a different timing that changes the picture.
Situation
Currently on SSRIs and don't want to taper
Ketamine does not interact with SSRIs. It is the most accessible option for people who are on antidepressants and either cannot safely taper or don't want to. Ketamine-assisted psychotherapy is available in all 50 states, is often insurance-covered as Spravato, and has strong evidence for treatment-resistant depression.
Find a ketamine provider →
Situation
History of psychosis in family, classics contraindicated
Ketamine again — its NMDA mechanism does not carry the same psychosis risk as 5-HT2A agonists. MDMA, with close monitoring and a clear psychiatric evaluation, may also be considered depending on the specifics. A psychiatrist with psychedelic expertise is the right person to evaluate this, not a general practitioner's conservative default.
Find a psychiatrist with psychedelic training →
Situation
Cardiac conditions that preclude MDMA/ibogaine
Psilocybin has a very mild cardiovascular profile and is typically accessible with stable cardiac conditions that would preclude MDMA or ibogaine. Oregon's licensed service centers can arrange physician consultation as part of the intake process. Ketamine also has a manageable cardiac profile in most cases.
Browse licensed psilocybin retreats →
Situation
Bipolar II, currently stable and off mood stabilizers
Bipolar II has a different risk profile than bipolar I. Some trials have included carefully screened bipolar II participants. This requires a detailed psychiatric evaluation with a provider who knows the psychedelic literature — not a standard psychiatric consult. The conversation should include: current polarity, history of hypomanic triggers, medication history, and support structure.
Find a psychedelic-informed psychiatrist →
Situation
On lithium for bipolar, can't come off it
Lithium and classic psychedelics are a genuine contraindication due to seizure risk. Ketamine does not carry this risk profile and remains an option. MDMA with careful cardiovascular monitoring may also be evaluated. This situation genuinely requires a psychiatrist who can model the tradeoffs, not self-navigation.
Ketamine options →
Situation
Not ready for a full session — want to start smaller
Integration therapy (working with a therapist on psychedelic-adjacent material without using substances) and preparation-only work are valuable on their own. Some people do several integration sessions before ever having a session, and some find that preparation work alone moves them significantly. This is not settling — it's building the foundation that determines outcomes.
Free integration toolkit →
What to ask
Questions a good provider should ask you — and that you should ask them
The quality of medical and psychological screening before any psychedelic session is itself a signal about the provider's competence. A provider who does not ask these questions is not doing adequate screening.
What a provider should ask you
1
Full psychiatric history — personal and first-degree family history of psychosis, schizophrenia, bipolar disorder, and mania
2
Complete medication list — including supplements, herbals, and as-needed medications, with doses and duration
3
Cardiovascular history — hypertension, arrhythmias, prior cardiac events, baseline ECG if relevant to the substance
4
Substance use history — current and past use of all substances including alcohol, and any history of dependence or problematic use
5
Suicidality assessment — current ideation, plan, intent; history of attempts
6
Current life circumstances — stability, support system, living situation, presence of safe people in your life
7
Intentions and expectations for the work — what are you hoping to get from this experience?
What you should ask the provider
1
What is your training in psychedelic therapy? Where, with whom, and how long?
2
How do you handle a difficult experience or psychological crisis during a session?
3
What is your protocol if I need emergency medical assistance?
4
How many preparation and integration sessions are included? What do they involve?
5
What is your policy on physical contact during sessions?
6
Are you licensed or certified by any regulatory body (Oregon OHA, MAPS, Fluence, etc.)?
7
What happens if I need support after the session? What's the follow-up protocol?
ℹ
Red flags in a provider: No medical screening beyond a brief form. Guaranteeing specific outcomes. Pressure to proceed quickly or minimize concerns. Physical touch without explicit consent. Not providing references or credentials. Discouraging you from discussing the work with your existing mental health provider. These are signs of inadequate or unsafe practice — not uncommon in the underground and retreat markets.
If you're in crisis right now
If you or someone you know is experiencing a psychological emergency related to a psychedelic experience, or any mental health crisis — reach out immediately.
Continue learning
Related guides
