If you're in crisis right now
Please reach out before anything else. These lines are staffed by people who understand military service and trauma.
Why veterans are turning to psychedelic therapy
PTSD and traumatic brain injury affect hundreds of thousands of veterans. The standard treatments — SSRIs, prolonged exposure therapy, cognitive processing therapy — help many people, but leave a significant portion without adequate relief. That gap is what's driving the research.
The VA's own data shows that fewer than half of veterans with PTSD respond adequately to first-line treatments. For those with treatment-resistant PTSD compounded by TBI — common among Special Operations veterans exposed to repeated blast events — conventional medicine has offered very little.
What makes psychedelic therapy different mechanistically is that it doesn't just manage symptoms — it appears to create a window of neuroplasticity that allows entrenched trauma responses to be restructured. For PTSD specifically, which involves rigid, hyperactivated fear memory networks, this mechanism may be particularly relevant.
This doesn't mean psychedelic therapy is a cure, universally appropriate, or without risk. It means the research signal is strong enough that the VA is now funding studies for the first time since the 1960s, bipartisan legislation is moving through Congress, and multiple well-funded nonprofits exist specifically to fund veteran access.
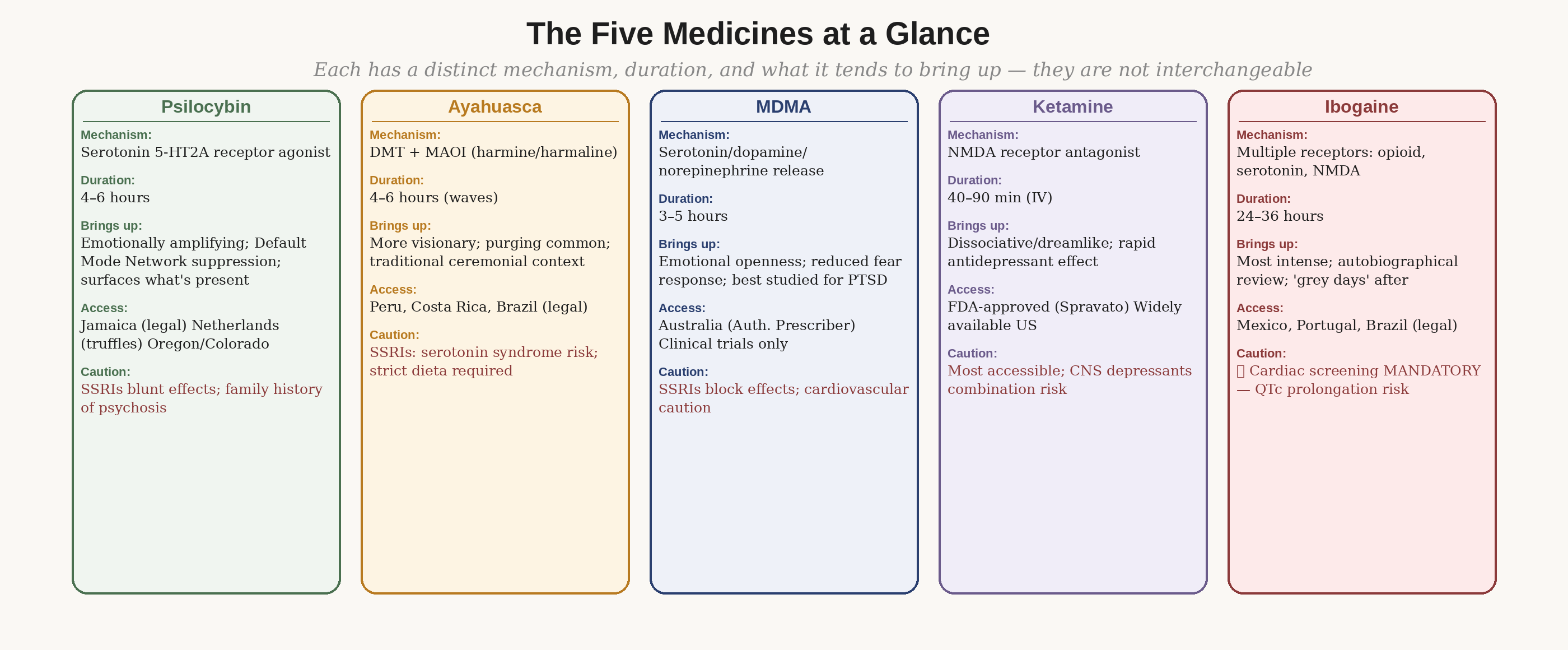
The five medicines compared — mechanism, duration, legal access, and key cautions. Each has a distinct profile.
The four medicines most studied for veterans
Not all psychedelics are equally studied or equally suited to the kinds of trauma veterans carry. Here's an honest breakdown of each.
Ibogaine has produced the most dramatic results specifically for the combination of TBI and PTSD that characterizes many combat veterans. The 2024 Stanford study in Nature Medicine showed 80%+ reduction in PTSD symptoms, with significant improvements in depression, anxiety, and functioning. A 2025 follow-up linked mystical experience intensity during treatment to better long-term outcomes.
The mechanism appears to involve a dream-like memory processing state that allows trauma to be reprocessed without the usual emotional overwhelm. Some researchers describe it as a neural "reset" — reducing the hyperarousal patterns associated with combat PTSD.
Access: Ibogaine is Schedule I in the US. Treatment currently requires traveling to Mexico (most common for US veterans), Portugal, or other international clinics. VETS Inc. and Mission Within specifically fund ibogaine treatment for veterans. Cost: $5,000–$18,000 depending on clinic.
MDMA-assisted therapy has the most Phase 3 clinical trial data of any psychedelic for PTSD. The MAPS Phase 3 trials showed significant improvements in PTSD symptoms — many participants no longer met PTSD diagnostic criteria after treatment. The FDA rejected the Lykos (formerly MAPS) application in August 2024 due to study design concerns, requesting an additional Phase 3 trial. This means MDMA therapy is not legally available in the US outside of clinical trials.
MDMA works differently from classic psychedelics — it reduces amygdala reactivity and increases oxytocin, making it easier to process traumatic memories without being overwhelmed by their emotional charge. Veterans describe being able to approach their most difficult memories without freezing or dissociating.
Access: VA-funded MDMA trials are now enrolling at multiple sites. These are free to participants. Australia has an authorized prescriber pathway active since 2023.
Psilocybin has the most research for depression and addiction, with PTSD-specific research still emerging. Texas funded a landmark veteran-specific psilocybin trial through HB 1802, led by Dr. Lynnette Averill, specifically for veterans with PTSD. Heroic Hearts Project has been among the first program partners for this trial.
Psilocybin's mechanism — 5-HT2A receptor agonism creating neuroplasticity — appears well-suited to disrupting the rigid fear memory patterns of PTSD. Research from Johns Hopkins has shown 80%+ abstinence rates for tobacco addiction and significant depression reduction in treatment-resistant cases. PTSD data is catching up.
Access: Oregon and Colorado licensed service centers are available now with no prescription needed. Clinical trials are enrolling. Heroic Hearts Project funds veteran psilocybin retreats internationally. Cost in Oregon: $1,500–$3,500 all-in.
Ketamine is not a classic psychedelic, but it produces similar neuroplasticity effects and is the most accessible option right now. Spravato (esketamine) is FDA-approved for treatment-resistant depression and is covered by most insurance including Tricare — making it financially accessible for veterans with coverage.
IV ketamine infusions are available off-label at clinics across the US and can produce rapid improvements in depression and PTSD symptoms. The VA has been studying ketamine for PTSD as part of its broader psychedelic research program. For veterans who need something now while other treatments aren't available, ketamine is a legitimate bridge.
Access: All 50 states via prescription. Spravato covered by Tricare with prior authorization. IV infusions $400–$800/session out of pocket. HSA/FSA eligible.
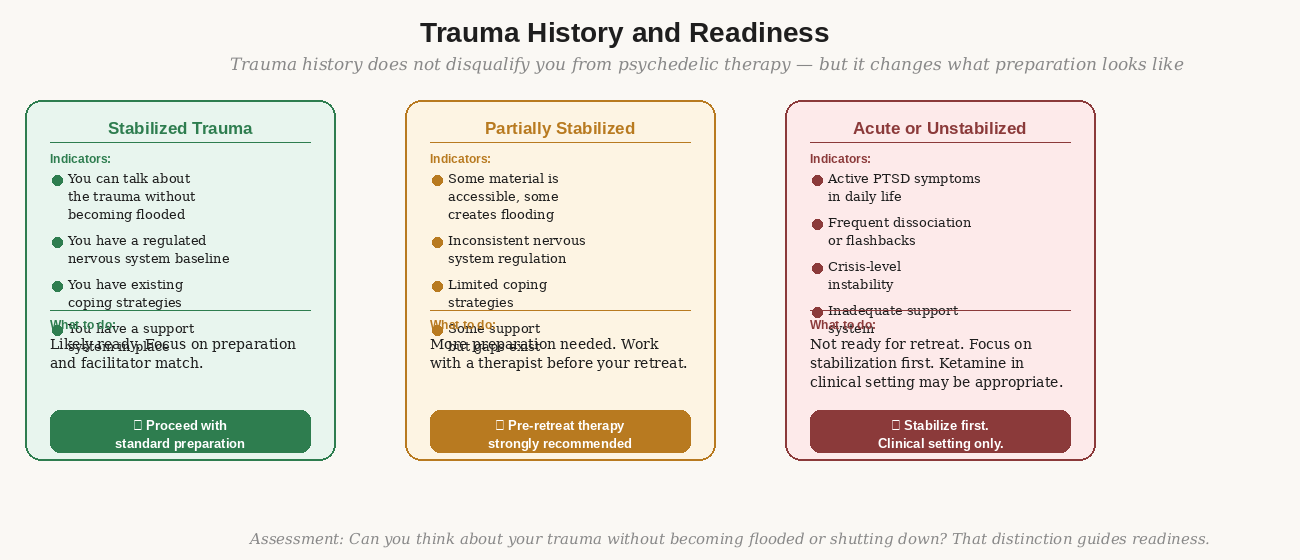
What trauma history means for session planning — what to disclose, and what a trauma-informed facilitator does differently.
How veterans actually access treatment
Access depends heavily on which medicine fits your situation and what you can afford. The pathways below are ranked from most accessible to least.
Organizations that fund veteran access
VETS Inc. (Veterans Exploring Treatment Solutions) Grants
Foundational Healing Grants covering ibogaine, psilocybin, MDMA, and ketamine — plus 5 one-on-one integration coaching sessions, weekly group coaching, and veteran mentorship. 1,200+ veterans funded since 2019. Applications currently paused; join the waitlist. vetsolutions.org →
Heroic Hearts Project Scholarships
Retreat scholarships on a sliding scale for veterans and veteran spouses. Covers ayahuasca, psilocybin, ibogaine, and ketamine treatments internationally. 800+ veterans served. Veteran spouses eligible through The Hope Project. Includes preparation, integration coaching, and peer community. heroicheartsproject.org →
The Mission Within Ibogaine specialists
Premier clinical psychedelic retreat provider for veterans. Specializes in ibogaine + 5-MeO-DMT for TBI and PTSD at medically supervised clinics in Mexico. 600+ veterans served. Grant funding covers most costs. Rigorous screening including cardiac clearance. Veteran underwriting program allows donors to sponsor specific veterans. missionwithin.org →
MAPS (Multidisciplinary Association for Psychedelic Studies) Research + referrals
Pioneered MDMA-assisted therapy research. Maintains a therapist integration list connecting veterans with MDMA-trained therapists. Actively conducting new Phase 3 trial following 2024 FDA feedback. maps.org →
VA Office of Research Development Clinical trials
Funding the first VA psychedelic studies since the 1960s — MDMA and psilocybin trials at VA medical centers. December 2024 announcement. Providence and West Haven VA sites enrolling for fiscal year 2025. Free to participants. research.va.gov →
Warrior Angels Foundation Ibogaine grants
Funds ibogaine treatment specifically for veterans with PTSD and TBI. Partners with medically vetted clinics. Application-based. Focuses on veterans who have exhausted VA treatment options. warriorangelsfoundation.org →
Active veteran-specific clinical trials
Clinical trials provide free treatment to participants who qualify. For veterans specifically, several trials are veteran-focused or veteran-preferred. All treatment, preparation, integration, and often travel expenses are covered.
The most comprehensive searchable database is at ClinicalTrials.gov. Search "veteran" combined with your condition and treatment type. VETS Inc. also maintains a curated list of active trials at their website. When evaluating a trial, check: location, eligibility criteria, time commitment, and whether travel expenses are covered.
Safety considerations specific to veterans
Veterans often have medical histories that require more careful screening than the general population — TBI, chronic pain medications, psychiatric medications, cardiovascular conditions from service. These aren't reasons to avoid treatment, but they're reasons to do the screening properly.
| Condition / factor | Ibogaine | MDMA | Psilocybin | Ketamine |
|---|---|---|---|---|
| TBI history | Well-studied — positive outcomes | Limited data — monitor carefully | Emerging data — positive signs | Some positive data for TBI cognitive effects |
| Cardiac issues / QTc prolongation | ❌ Contraindicated — ECG required | Caution — cardiovascular monitoring needed | Generally safe — low cardiac risk | Caution — BP monitoring needed |
| SSRIs / antidepressants | Must taper off — serious interaction risk | Must taper off — serotonin syndrome risk | Taper recommended — reduces effect | Generally compatible — discuss with prescriber |
| Opioid use / addiction history | Strong anti-addictive evidence | Caution — discuss with clinician | Positive data for addiction generally | Use caution — addiction potential |
| MST (Military Sexual Trauma) | Discuss with facilitators — trauma-informed setting essential | MDMA specifically studied for trauma — good fit with proper support | Can surface difficult material — preparation essential | Lower intensity — may be better starting point |
| Dissociation history | Discuss with clinicians — high-intensity experience | Generally manageable with proper support | Discuss with facilitators — preparation key | Can cause dissociation — screen carefully |
| History of psychosis / schizophrenia | ❌ Contraindicated | ❌ Contraindicated | ❌ Contraindicated | ❌ Contraindicated |
Policy landscape & VA developments
The policy environment for veteran psychedelic therapy has shifted dramatically in the past two years. Here's the current state.
Federal — 2024–2025
December 2024: The VA announced $1.5M in funding for MDMA and psilocybin studies — the first time the agency has directly funded psychedelic research since the 1960s. This is a significant institutional shift.
2025: Representatives Correa and Bergman introduced the Innovative Therapies Centers of Excellence Act — bipartisan legislation to create dedicated VA research centers studying MDMA, ibogaine, ketamine, and psilocybin for PTSD, TBI, depression, and addiction. Endorsed by the American Legion, DAV, IAVA, VFW, and Wounded Warrior Project.
State level
Texas: Governor Abbott signed legislation requiring the state to study ketamine, psilocybin, and MDMA for veteran treatment. UT Austin Dell Medical School launched the Center for Psychedelic Research and Therapy as a direct result.
Oregon and Colorado: Licensed psilocybin service centers are operating now. Veterans can access these without a prescription, physician referral, or documented diagnosis — the lowest-barrier legal domestic option currently available.
What's still missing
No federally approved psychedelic therapy for PTSD yet. MDMA therapy's FDA rejection in August 2024 delayed that by several years. Ibogaine remains Schedule I with no formal FDA pathway currently, despite the strongest veteran-specific evidence. The VA cannot prescribe or administer these treatments — veterans still need to travel internationally or access state-licensed programs for most options.
